Pressure Ulcer Prophylaxis – Prevention Of Pressure Sores
It is essential to change the patient’s position frequently in order to prevent pressure sores, which can occur when sustained pressure is applied to an area of skin.
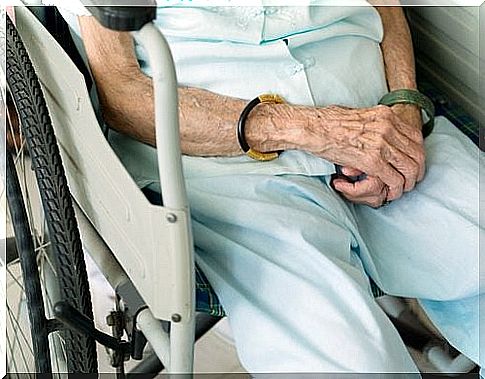
The pressure ulcer prevention is very important to prevent bedsores when one is captivated by a disease or by the age of the bed or to a wheelchair and can hardly move.
The same areas of skin are continuously exposed to pressure, which leads to reddening of the skin and pressure sores.
To avoid this, various prophylactic measures are required, which we will explain in more detail below.
What are bedsores?
In patients who are bedridden for a long time, tissue damage can occur over time, as certain areas of the skin are constantly stressed and the blood circulation is disturbed as a result.
The resulting wounds can cause great pain and further increase the restricted mobility of the affected patient.
The pressure exerted by the bones against the mattress or pillow causes uncomfortable wounds, especially in those areas where the soft tissue coverage is low but the bones are prominent.
In some cases, moisture also plays a role, which can make the problem worse, for example if the person has urinary incontinence.
The wounds are divided into four different degrees of severity depending on the extent of the damage.
Initially, the skin is reddened, but in the advanced stage, deeper tissue structures such as muscles, bones and tendons are affected.
The bedsores can also cause infections that cause great suffering and can get worse if the person’s position is not changed.
The following risk factors increase the risk of pressure ulcers:
- advanced age
- complete immobility
- Urinary incontinence or lack of control of the excretory system
- Malnutrition or dehydration
- slow healing diseases
- mental disorders (dementia, confusion, Alzheimer’s)
- sedative medicines
What measures are taken for pressure ulcer prophylaxis?
This problem is particularly common in older people who are bedridden for a long time. Both nurses and relatives of these patients should take care that bedsores do not develop in the first place.
The following tips can help preventively:
1. Change the position every 2 to 3 hours
Depending on the possibilities of the patient, this should be rotated regularly so that the blood circulation is improved and the pressure does not always stress the same areas.
- Pillows can be used to support the back and turn the patient to one side or the other.
2. Monitor vulnerable areas
Certain areas of the body are particularly sensitive because the soft tissue coverage is low: heels, hips, sacrum, knees, ears and shoulders.
If there is reddening of the skin, it should be treated as soon as possible to avoid pressure sores.
3. Proper personal hygiene
Even if the affected person is always in bed, the body becomes contaminated by perspiration and other circumstances. Proper personal hygiene or (if possible) taking a shower every day are essential to reduce the risk of sore ulcers.
- Use neutral soap without rubbing the skin heavily.
- Drying off is also very important in decubitus prophylaxis, because moisture promotes reddening of the skin.
4. Reduce pressure points
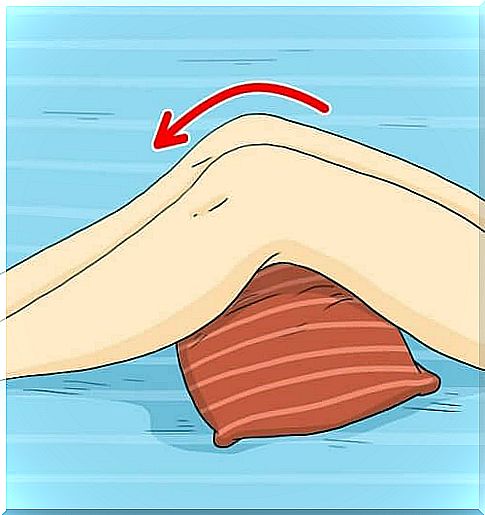
By using pillows or special aids, you can bed the patient or put them in the wheelchair so that there are fewer pressure points.
- For example, if your legs are putting pressure on each other, you can place a pillow between your knees.
- There are several tools that can be of great use in these cases.
5. Good nutrition and adequate water
A balanced diet, which must be adapted to the individual needs of the sick person, is fundamental to improve general well-being and prevent complaints.
In addition, plenty of water, teas and soups are recommended. Also, gelatin is very important to ensure a aureichende liquid supply.
6. Prevent pressure on the heels
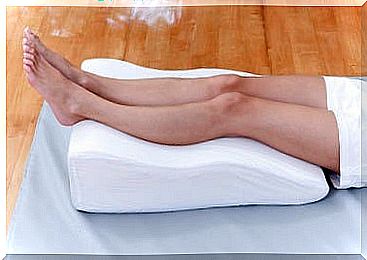
You can place a special pillow under the calves so that your feet are loosely in the air without putting pressure on them.
It is also important that the sheets are as airy and loose as possible.
7. Massage as pressure ulcer prophylaxis
The affected person should be massaged two to three times a day to improve blood circulation and avoid numbness in the muscles.
Use a special lotion or ointment for this.
However, prominent bones should not be massaged, because the additional pressure could damage the fine layer of skin (for example on the knee).
8. Replace sheets
Make sure the sheets are adequate and replaced regularly.
- They should not be too tight, but also not too loose so that the skin can breathe easily, but the sheet does not wrinkle and exert additional pressure.
- The bed linen should not have buttons, zippers or thick seams.
- It is also important to change the sheets and air them regularly to prevent moisture and dirt.
9. Exercises to prevent pressure ulcers
If the patient is unable to move on their own, it is important to regularly passively move their legs, arms, neck, and other parts of the body.
This can improve blood circulation and at the same time reduce the pressure against the bed.
Natural remedies for the treatment of mild pressure sores
These home remedies can only be used in mild cases. You should definitely always seek the advice of an expert on treating ulcers.
1. Aloe vera

You can buy aloe gel or cut a fresh leaf to remove the gel. This cools the skin and improves blood circulation.
In addition, aloe vera helps prevent infection and brings immediate relief.
2. Milk of magnesia
You can buy magnesia milk in the pharmacy. This can reduce skin redness and swelling. Apply this remedy to the sore area with cotton wool three times a day.
3. honey
The antibacterial properties of honey are of great help in treating newly formed pressure sores. Honey also provides moisture to the skin.
Simply apply some honey and cover with a bandage.